Table of Contents
If you or someone close to you has ever experienced red, painful skin, with a glossy and swollen appearance, then you know what we are talking about today. Yes, you are correct – today’s topic is cellulitis, this famous skin condition that raises multiple questions when it comes to causes, methods of prevention, and treatment.
However, if you haven’t heard about this condition, the first distinction to be made is that cellulitis is nothing like cellulite. Although they both affect the skin, which is the largest organ on the body, cellulitis is a bacterial infection and, therefore, requires more attention and treatment. On the other hand, cellulite forms bumps and dimples on the skin without causing any pain. Commonly found in the buttock and thighs areas, cellulite is due to fat deposits pushing through the connective tissue underneath the skin.
Since there are several misconceptions about cellulitis, we will share what is important for you to know about this inflammation of the skin in this article.
So, let’s start with some common questions.
What is Cellulitis?
Cellulitis is a bacterial skin infection. Although statistics indicate that it is relatively common, one can never be sure because it generally goes without being reported. Even though cellulitis can occur at any age, individuals 45 years or older are at increased risk. The elderly too are especially susceptible to developing cellulitis.

How does cellulitis manifest? The skin that is affected by cellulitis is usually red, swollen, and warm to the touch. If you are wondering how you can tell the difference between cellulitis and a simple insect bite, trust me, you will easily spot the difference.
Cellulitis is much more unpleasant and painful than a mosquito or spider bite.
Medicinenet.com states, cellulitis can often be mistaken for stasis dermatitis, a skin condition caused by poor circulation, which has similar symptoms. That is why we highly recommend visiting your doctor and getting properly diagnosed.
So, how can you get cellulitis? Well, there are several causes of cellulitis. From the beginning you should know, cellulitis does not discriminate. It can affect people of all ages and races, men and women alike. However, statistically, it is more prevalent in middle-aged and older persons.
All these questions lead us to one of the most asked: is cellulitis contagious? No, cellulitis is not contagious by itself as the infection involves the deep skin layers, while the top layer of the skin still intact provides a barrier.
Before reading further, please remember that cellulitis can spread to the bloodstream or to lymph nodes. That being said, cellulitis is just like any other infection – if it is not treated, it can become life-threatening. That is why it is important to be well informed about it.
Causes
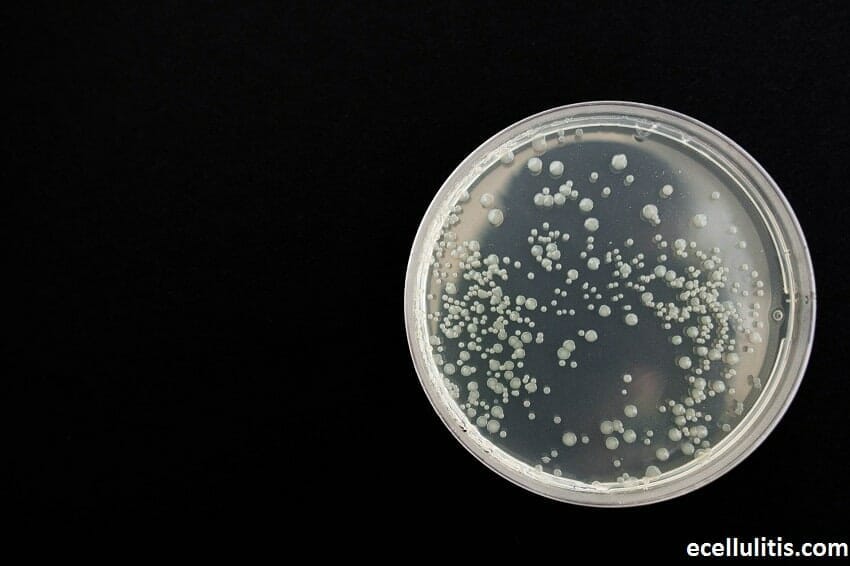
Streptococcus and Staphylococcus are the pathogens more frequently associated with cellulitis. Infection occurs when these microorganisms that normally reside on the skin penetrate the protective barrier; this may happen anywhere on the body, but the leg seems to be the preferential location for this bacterial infection.
Depending on which pathogen enters the tissue, there are different types of cellulitis. For example, erysipelas is caused by the Strep and is manifested as a bright, red, hot area on the skin. This sort of cellulitis is most commonly found in children.
There are several types of cellulitis:
- Breast cellulitis
- Facial cellulitis (most commonly found on cheeks or nose)
- Periorbital cellulitis (affecting the region around the eyes)
- Perianal cellulitis which occurs around the anal orifice
Bacteria can enter the skin through abrasions, blisters, burns, or insect bites. They may also appear in conjunction with skin disorders such as eczema and athlete’s foot.
Drugs that suppress your immune system increase your risk of cellulitis. These are usually medications used to prevent organ graft rejection, treat autoimmune disorders and other inflammatory conditions, such as asthma and psoriasis.
Your chances of getting cellulitis increase if your immune system is weakened.
Pregnancy, obesity, diabetes and other conditions that reduce your blood circulation, also make you susceptible to cellulitis.
Are There Any Other Causes of Cellulitis?
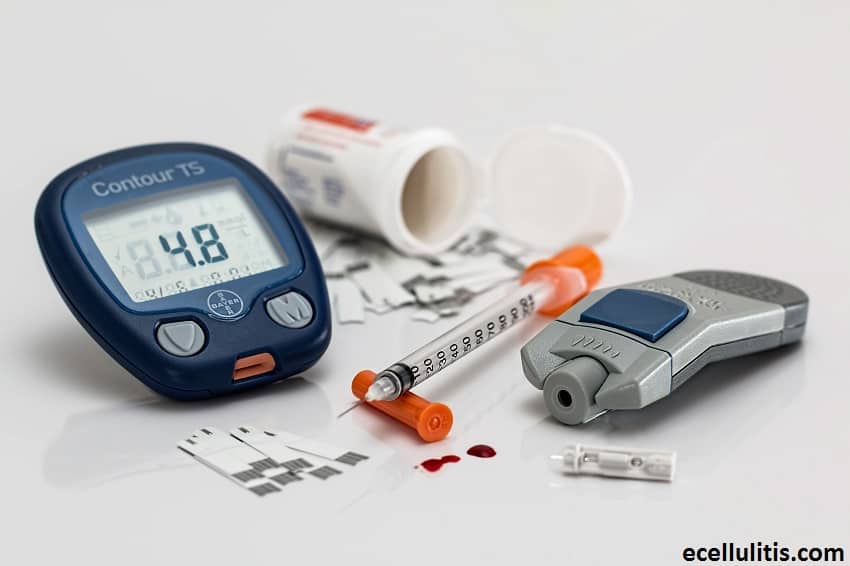
Yes, there are. In fact, multiple bacteria can cause this infection. For example, according to Medicine.net, Haemophilus influenzae bacteria is frequently responsible of cellulitis in infants and children under 6 years of age. The list only goes on with bacteria that can be transmitted from animals, or even from contaminated fresh or seawater.
Other not so familiar causes of cellulitis are poor blood circulation and diabetes. Poor circulation can affect the body’s ability to protect itself from infections. Poorly controlled diabetes weakens the immune system, which automatically makes you susceptible to cellulitis.
The improper use of needles is another route for penetration of the infection. For example, intravenous drug users are prone to develop cellulitis as they tend to use the same needle over and over again.
Symptoms of Cellulitis
Cellulitis is inflammation in the subcutaneous tissue. This is the layer beneath the skin’s surface. The affected lower dermis layers propagate the inflammation to the underlying connective tissues.
The symptoms of this condition include swelling, warmth, redness, and tenderness or pain in the infected area. Other general symptoms are fever, chills, sweating, and fatigue. Patients can also experience pain and joint stiffness. The most commonly infected areas include the lower portion of the legs, arms, neck, and head.
The infection can migrate to the lymph nodes and cause them to swell. If the infection reaches the bloodstream, it can cause life-threatening complications.
How to Diagnose Cellulitis?
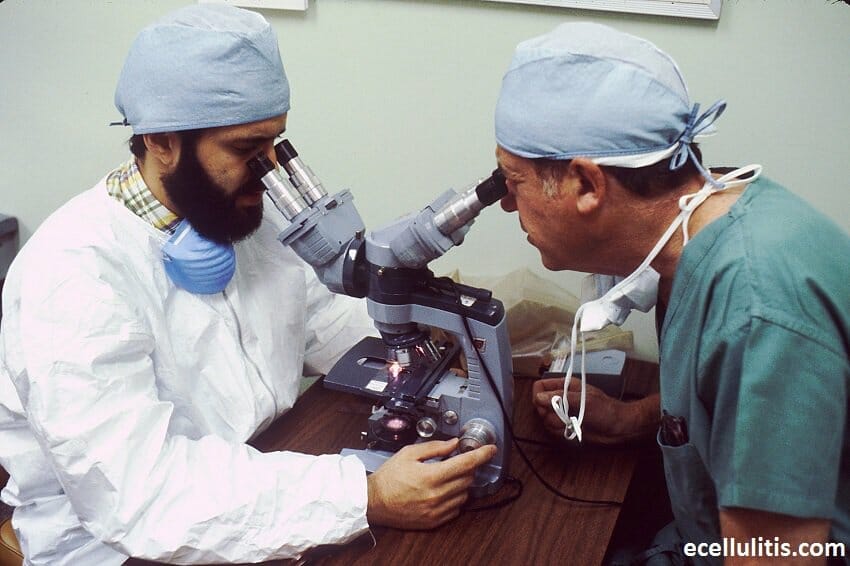
A doctor will perform a physical examination and document the patient’s medical history. During the exam, the doctor will check the patient for symptoms commonly associated with cellulitis. The physician may request a full blood panel aimed at assessing bacterial infection. Usually, an elevated white blood cell count raises red flags and will help diagnose the infection.
Chances are you will be able to recognize cellulitis on your own. However, it is always recommended to seek professional advice to receive appropriate care.
In some cases, your doctor may not provide a prescription immediately after the first appointment but a follow-up instead to see whether or not the swelling and the redness spread. However, if you are experiencing severe pain and high temperature, you should inform your doctor, and he/she will ensure you receive the appropriate treatment without delay.
Treatment
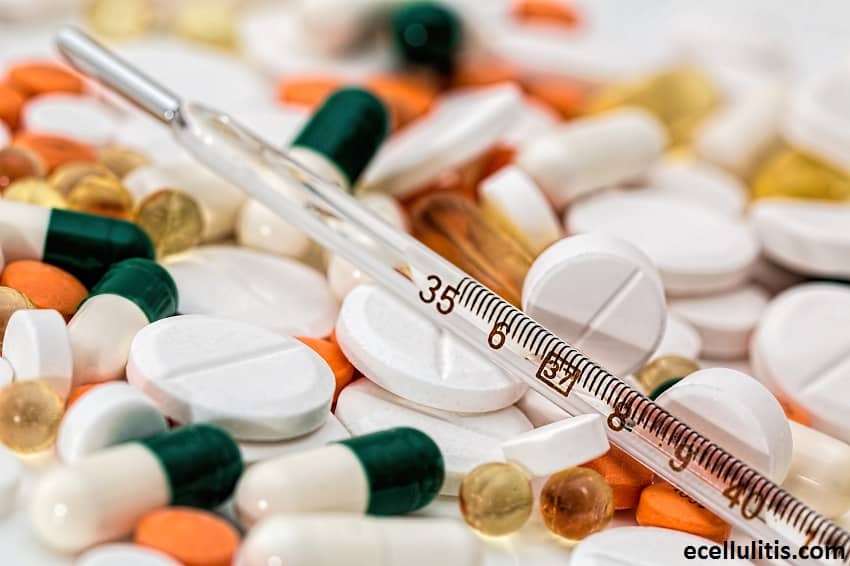
The primary treatment for cellulitis relies on the administration of antibiotics. These medications may be derivatives of penicillin or other types of antibiotics that are effective against streptococcal and staphylococcal infections. The good news is that many antibiotics can be used to treat cellulitis.
If the infection is severe, it may require hospital admission and intravenous injection of antibiotics. The location and extent of the infection, along with your medical history, will also help determine the appropriate treatment for your condition.
How long should you take antibiotics? The answer depends on your general status and the severity of the cellulitis. The most common are 10-day or 21-day regimens of antibiotics. The first effects of antibiotics are usually seen a couple of days after the beginning of the medication. That said, the crucial part of treating this inflammation is to be consistent: if your condition is starting to improve that doesn’t mean you should stop taking antibiotics. If you are experiencing too much pain, you may also need pain relievers.
In cases where cellulitis symptoms are serious such as high fever, no improvement or worsening after a course of antibiotics, high blood pressure, diabetes, or other risk factors, your doctor will suggest hospitalization.
Why is it So Important to Treat Cellulitis?
How serious is cellulitis? This condition should not be neglected as it may lead ultimately to life-threatening complications. Permanent damage to the lymphatic system, and sepsis or septicemia are the most significant complications of cellulitis.
In addition to permanent damage, cellulitis may cause to the lymph vessels due to long-standing inflammation, we should mention some specific conditions such as gangrene, blood and bone infection.
Gangrene
Gangrene, or tissue death, occurs when a tissue is not getting enough blood from the circulatory system. It typically starts with a certain part of the body, like leg and arm, but can also affect internal organs. Why is gangrene life-threatening? The answer is simple – if not treated properly and on time, it can cause the body to go into shock, which is a medical emergency.
The good news is that gangrene is easily spotted. If you notice that the wound is becoming dark red, sore, and gives off a bad smell, while your whole body feels cold, be sure to rush to the emergency room.
Blood and Bone Infection
Blood infection, septicemia or blood poisoning, is a condition in which a bacterial infection gets into the bloodstream. What makes septicemia dangerous is that the toxins are carried throughout the entire body. As a result of the general propagation of the infection, organs start to fail.
Bone infection or osteomyelitis occurs secondarily to the spread of bacteria into the bloodstream. This complication can occur suddenly, or remain asymptomatic for a long time. Moreover, it is well known that only a few antibiotics can easily penetrate bone structures. If you want to find out more about this condition, be sure to check the Healthline.com article on this matter.
Inflammation of the Lymph Vessels in the Affected Region
The lymphatic system consists of lymph vessels and lymph nodes. Lymph nodes are small organs containing immune cells. These cells protect you from viruses and other types of pathogens. Lymph nodes in the armpits, neck, and groin are easily accessible for examination.
The presence of enlarged or swollen lymph nodes can be a sign that the infection is spreading to the lymphatic system. This is commonly diagnosed during physical examination. So if you have any suspicions be sure to consult a physician.
Please remember that all of the stated conditions can be fatal if not treated on time.
Prevention

Practicing good hygiene, wearing protective clothing, treating wounds, can prevent many cases of cellulitis. I can’t emphasize enough the importance of good hygiene. Be sure to keep an eye on your skin and moisturize regularly, if you notice your skin is cracked or dry. This is especially important during fall and winter when the skin is naturally drier than usual.
Here’s another tip: Be sure to clean and care adequately for a wound as soon as it is inflicted.
On the other hand, if you are predisposed to developing the condition, or have a weakened immune system, you may not be able to prevent the disease.
For people with healthy immune systems, safeguarding the skin is the best way to prevent cellulitis. If you are looking for a way to boost the immune system and prepare your body for the fall, be sure to get your hands on this article I wrote a year ago.
Let’s Recap!
Here are a few takeaways about cellulitis:
- Cellulitis is a deep bacterial skin infection. It can affect people of any race and age, although it is most commonly found in people over 45 years old.
- It manifests as red, swollen skin that is usually warm to the touch. The affected area appears “glass-like” and extremely tight. There is an obvious difference between cellulitis and insect bites – cellulitis is far more painful.
- Multiple bacteria cause cellulitis, two of them being streptococcus and staphylococcus.
- There are several types of this condition depending on where it is located.
- There are many causes of cellulitis, the most prominent is having a weakened immune system. Also, cellulitis can be triggered by eczema, obesity, pregnancy, diabetes, etc.
- There is more to cellulitis than just red, painful skin. Other associated symptoms are fever, chills, sweating, and fatigue.
- Cellulitis is not contagious but can be life-threatening.
- To get diagnosed properly, be sure to visit your physician. Cellulitis is treated with different types of antibiotics, depending on which bacteria caused it. Your body should respond pretty quickly to medications. If that is not the case, hospitalization may be indicated.
- Can cellulitis be prevented? Yes, of course! Practice good hygiene, eat a well-balanced diet to boost your immune system, moisturize your skin, and if you have a chronic skin disease, seek a health practitioner to ensure proper management.
Have you or maybe someone close to you ever had cellulitis? What was your experience, and how long did it take you to recover? Share your thoughts with Ecellulitis community in the comment section below!
Image credit: DepositPhotos.com
Last article update: 9/22/2018
Medically reviewed by Dr. Thouria Bensaoula on Sept 18, 2019.
