
Table of Contents
- 1. Osteomyelitis (bone infection)
- 2. Meningitis (brain and spinal cord infection)
- 3. Lymphadenitis (inflammation of the lymph nodes)
- 4. Abscesses (pus collection)
- 5. Sepsis (the infection has spread to the whole body, also known as septic shock)
- 6. Thrombophlebitis (vein inflammation complicated with thrombosis)
- 7. Necrotizing Fasciitis (an infection that leads to the destruction of the tissues surrounding the muscle, nerves, vessels under the skin)
- 8. Gangrene (tissue death)
- 9. Recurrent cellulitis
Cellulitis is an infection of the dermis and subcutaneous tissue mainly caused by bacteria. Common symptoms are redness of the affected area, inflammation, swelling, pain, chills and fever.
This type of infection is most commonly found on the extremities (legs and arms) in adults, or the face in children (periorbital type).
Cellulitis may rapidly spread. Because of that, it is fundamental to consult with your GP or another medical professional as soon as symptoms arise, to avoid serious cellulitis complications, which can be sometimes life-threatening.
According to medical literature, cellulitis can lead to the following complications:
1. Osteomyelitis (bone infection)
Osteomyelitis is a serious bone infection that commonly originates from another part of the body and is transported to the bone through the blood.
Symptoms of this infection may include: bone pain, swelling, redness and warmth in the affected region, fever, general discomfort or malaise. Other associated symptoms are chills, sweating and diffuse lower back pain.
2. Meningitis (brain and spinal cord infection)
Meningitis an inflammation of the membranes covering the brain and spinal cord, also known as the meninges.
This complication may occur in cases of neglected facial cellulitis. Bacterial meningitis is a severe condition that needs to be managed as a medical emergency. It can result in brain damage and long-term debilitating conditions such as epilepsy, for example, even when the patient has been adequately treated.
In most cases of meningitis, symptoms develop rapidly and may include: photophobia (intolerance to bright light), neck stiffness, severe headaches, chills and fever, nausea and vomiting. These signs are often accompanied with mental status changes.
3. Lymphadenitis (inflammation of the lymph nodes)
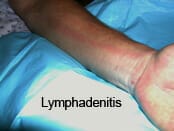
Infection of the lymph nodes (or lymphatic glands) is known as lymphadenitis. It manifests as a swelling of the lymph nodes, located in the territory of the affected skin. This means that the inflammatory reaction that started in the deep skin layers has spread to the lymphatic nodes. Lymphadenitis is a common finding in bacterial and viral infections.
Lymphadenitis may progress into the formation of an abscess; in this case, lymph nodes may feel rubbery, softer to the touch, and the overlying skin may feel warm and red.
This condition may spread within hours. Therefore, a visit to a doctor is strongly advised and treatment should start as soon as possible.
4. Abscesses (pus collection)
 An abscess is a collection of dead inflammatory cells and white cells (neutrophils), as a reaction to the presence of bacteria. Also known as skin boils, these abscesses can appear as lumps raised above the skin’s surface, causing pain and swelling.
An abscess is a collection of dead inflammatory cells and white cells (neutrophils), as a reaction to the presence of bacteria. Also known as skin boils, these abscesses can appear as lumps raised above the skin’s surface, causing pain and swelling.
This condition sometimes requires professional medical attention. The doctor will drain and pack the area to help the healing and prevent infection.
5. Sepsis (the infection has spread to the whole body, also known as septic shock)
Sepsis is a severe complication in which the bloodstream is overwhelmed by bacteria. Bacteria can then migrate anywhere in the body.
Most usual places where an infection might spread include: The tissue covering the bowel (peritonitis); the kidneys (pyelonephritis); the lining of the brain (meningitis); the liver or the gall bladder; the lungs (pneumonia); the deep layers of the skin (cellulitis).
In a state of sepsis, blood pressure drops, resulting in a shock. Major organs and body systems, including the kidneys, liver, lungs, and central nervous system stop working properly. A change in mental status and hyperventilation may be the earliest sign of sepsis.
The manifestations of sepsis may vary with the age of the individual and his/her previous general health status. As an example, old patients with chronic diseases or infants, may present hypothermia instead of fever, which otherwise is a reliable sign of infection.
Other symptoms of sepsis include confusion or delirium, chills, light-headedness due to low blood pressure, rapid heartbeat, shaking, warm skin and sometimes a skin rash.
6. Thrombophlebitis (vein inflammation complicated with thrombosis)
Cellulitis can impede deep venous circulation, most frequently in the leg area, resulting in thrombophlebitis. This condition leads to the formation of blood clots within a deep vein; the clots can migrate to the lungs or the heart and cause life-threatening complications.
Individuals who experience cellulitis in the legs are often prescribed blood thinners or special stockings to prevent venous stasis, clot formation, and promote circulation. On a preventive side, regular physical activity such as walking, is recommended in individuals with poor venous circulation.
7. Necrotizing Fasciitis (an infection that leads to the destruction of the tissues surrounding the muscle, nerves, vessels under the skin)
Also known as “flesh-eating bacteria”, necrotizing fasciitis, is thought to be mainly caused by a group A Streptococcus.
The first symptoms of necrotizing fasciitis include a red or swollen area of skin that spreads quickly, a severe pain that goes beyond the affected skin, and fever. Le lesion will progress later into a blister, a black, bronze or purple spot, which can break open with pus.
Dizziness, tiredness and nausea may be associated to local signs.
This strong inflammation causes tissue death (necrosis) and irreversible damage to the tissues. This is a very serious condition, which mandates urgent hospital admission and intravenous administration of antibiotic combined to surgery.
8. Gangrene (tissue death)
Gangrene occurs when blood flow is restricted in an area of the body; this results in the death and decay of otherwise healthy tissue.
Tissue death may be the result of a severe infection, injury or vascular conditions. Gangrene can spread quickly, so it requires urgent surgery to remove dead tissue. It may be prevented most of the times if cellulitis has been properly managed to avoid irreversible tissue damage.
9. Recurrent cellulitis
Studies have shown that as many as 45% of affected individuals may experience a recurrence of cellulitis within 3 years.
Individuals with a weakened immune system or a chronic condition, such as poor venous circulation, fungal infections, diabetes, lymphedema, advanced age, are more prone to this type of complication.
For prevention of recurrence, it is crucial to frequently observe previous cellulitis sites for potential signs of reinfection, treat underlying conditions such as fungal infections, and prevent dry skin.
Image credit: DepositPhotos.com
Last article update: 10/4/2019
Medically reviewed by Dr. Thouria Bensaoula on Oct 03, 2019.
